Hemoglobin, (Hb) is the oxygen-carrier protein found in Red Blood Cells. Hemoglobin consists of four helical polypeptide chains (two alpha chains and two beta chains) and four heme groups.
Biochemistry
Each of the four chains, folds around and shelters a porphyrin ring that has an iron atom at its center. Oxygen binds to the iron. The porphyrins rings and their irons are known as heme groups, and they are responsible for the red color of blood.
The alpha chains are identical and have 141 amino acids each, the beta chains are identical and have 146 amino acids each.
It is the replacement of the amino acids, at position 6 on the beta chains that leads to abnormal hemoglobin and sickle cell diseases.
Glutamic acid is the amino acid that normally occupies the 6th position on the beta amino acids chains. Normal hemoglobin A (Hb-A), has glutamic acid occupying the 6th position on the beta chains.
In Hb-S, valine is the amino acid found at position 6 on the beta chain of amino acids.
In Hb-C, lysine is the amino acid found at position 6 on the beta chains of amino acids.
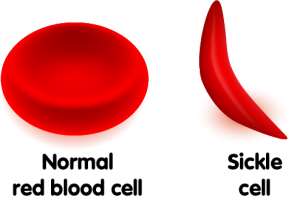
In the absence of oxygen, and in acidic environment, the Hb-S chains join together to form long chains that distort the shape of their RBC membranes, leading to the formation of rigid, sickled shape (banana-shaped) RBCs.
The sickling of RBCs leads to two major problems.
.1) The sickled RBCs become rigid and sticky. As they travel through small blood vessels, they get stuck and clog the blood flow.
Clogging may cut-off the blood supply to various tissues and organs in the body causing pain infections and even strokes.
. 2) The sickled RBCs have a shortened lifespan. They are prone to being swallowed by macrophages (special type of WBCs) and/or getting destroyed by the Spleen. This leads to persistent hemolytic anemia.
The lifespan of normal RBCs is about 115 days. The lifespan of Hb-S RBCs is 10-20 days.
GENETICS
About 1.9% of newborn babies in Ghana carry two sickle cell genes (“S”) one from each parent. Homozygous Hb-SS, is the severest form of sickle cell disease
About 30 % of Ghanaians have the sickle trait, they carry one “Hb-S” gene and one normal “Hb-A” gene. They are said to be heterozygous. Hb AS.
The Hb-S gene may be inherited from either parent in an autosomal recessive pattern
If both parents carry the sickle trait, that is, if both parents have Hb-AS genes, then with each and any of their pregnancies, the child born to them, shall have
. 25% chance of inheriting 2 “Hb-S” genes, the Hb-SS, one from each parent (full-blown sickle cell anemia)
. 25% chance of inheriting two normal genes, the Hb-AA (normal)
. 50% chance of inheriting one “S” and one Normal “A” gene, the trait: Hb-AS (sickle trait)
In those with sickle traits, about 40% of their hemoglobin is Hb-S and 60%, Hb-A.
SICKLE CELL TRAIT AND MALARIA PARASITE (Plasmodium falciparum).
Plasmodium falciparum, the malaria parasite, may enter any RBC. When it enters Hb-S type of RBCs, it triggers sickling formation in those RBCs.
The sickled cells are either rapidly swallowed by macrophages or destroyed by the spleen. The term suicidal infection has been used to describe this phenomenon.
This suicidal infection helps children with the sickle trait, (Hb-AS), and who are less than 5 years of age, to eliminate the malaria parasite from their bodies, and to withstand severe malaria infections until they develop full resistance to severe malarial infection, later on.
So young children, under 5 years with the sickle trait, (Hb-AS) have the advantage in fighting off severe malaria infections, compared to their cohort who are either Hb-AA or Hgb-SS.
Actually, those with Hb-SS perform poorly and are highly susceptible to the lethal effects of malaria infections.
It is estimated Hb-AS provides 60% protection against Malaria Deaths in children 2-16 months old (1)
MANIFESTATIONS AND COMPLICATIONS OF SICKLE CELL DISEASES.
Symptoms of sickle cell diseases, are delayed until the child is 6-12 months old. Newborn babies and infants do have high levels of fetal hemoglobin, Hb-F, in the circulation. Hb-F, retards sickling formation.
Swelling of the hands and feet in an infant is the first symptom of Hb-SS. It is due to sickled RBCs blocking blood flow in and out of the hands and feet.
This condition is treated with fluids and pain medicines.
The markers of sickle cell diseases are:
. Hemolytic Anemia (RBCs destruction leading to anemia)
. Painful occlusion of blood vessels
. As a result of frequent cut in blood supply, there are multiple microscopic areas of tissue death, microinfarcts, in many organs, including the Brain, Spleen and Kidneys.
Sickle cell complications can occur in any organ system and lead to severe decrease life expectancy.
. (I) PAINFUL EPISODES
Painful episodes are characteristics of Sickle cell diseases. Pain may be acute or chronic.
Pain results from cut of blood supply to the affected areas.
PRECIPITATING FACTORS:
. Sudden change from Warm to Cold Weather (leading to vasoconstrictions)
. Dehydration (from exertion or working out in the sun, when the weather is hot)
. Infections
. Alcohol intoxications
. Physical and Emotional stress
. Comorbidity: Pregnancy, Asthma, Sleep apnea, Acidosis
Acute pain requires: Narcotic analgesics, rehydration, warmth, NSAIDs and adequate rest
AVOIDANCE OF PAINFUL EPISODES:
. Drink plenty of fluids
. Try not to get too hot or too cold.
. Avoid high altitudes, and places with low oxygen levels
Acute Hepatic Crisis
Due to vaso-occlusive sickling episodes in the liver, a person may develop sudden liver enlargement, elevated liver enzymes, and pain in the liver area.
The right upper quadrant abdominal pain does not last long, but this condition must be distinguished from the associated Liver sequestration crisis.
Sequestration Crisis
Sequestration occurs when large number of sickle cells get trapped in the Spleen or Liver, causing these organs to enlarge. Sequestration is characterized by the following:
Signs: Liver and or splenic enlargement (Splenic sequestration) and. Rapid fall in Hemoglobin levels
Symptoms: sudden weakness, pallor, fast breathing, fast heartbeats, extreme thirst and abdominal pain.
Sequestration crisis is treated with Blood transfusion and Exchange transfusions to improve the anemia
Acute Chest Syndrome (ACS)
This condition is due to vaso-occlusion in the lung circulation. The Hb-SS person develops sudden
. Chest pain. Fever with temperature> 101.3F. Fast breathing. Wheezing. Cough
. Chest X-ray shows infiltrate in one or more lung segments.
ACS is treated in the Intensive care, with Oxygen, taking deep breaths, Antibiotics and Exchange blood transfusions
. (ii) HEMOLYSIS
Sickle cell disease is associated with RBC destruction and perpetual anemia. Most sickle cell RBCs, survive only 10-20 days.
The end products of hemolyzed RBCs: free Hemoglobin and Arginase, are toxic to the inner linings of small blood vessels, they lead to destruction and narrowing of blood vessels. Arginase degrades Arginine, the substance required to form Nitric oxide. Nitric oxide opens up small blood vessels, and in its absence, the vessels collapse, and free radicals pile up.
Hgb-SS persons are prone to develop Pulmonary Hypertension, due to free plasma Arginase.
The short lifespan of sickle RBCs, cause the bone marrow to overwork, to produce more RBCs. There is bone marrow hyperplasia in all the skeletons.
. (Iii) MICROINFARCT
Spleen
Recurrent microinfarct in the Spleen, due to frequent cuts in blood supply, destroys the spleen’s ability to fight infections. Hb-SS persons are susceptible to Pneumococcus, H. influenzae, Salmonella, Mycoplasma and E. coli infections
Brain
Sickle cell disease Children are at risk for Ischemic stroke during their childhood, and as they advance in age.
About a third of sickle cell disease persons have silent brain infarcts.
In children (2-16 years) Annual intracranial doppler Ultrasound of the Middle Cerebral Artery, is done to assess the flow velocity and predict the risk of a stroke.
Transfusions to decrease Hb-S level<30% prevents stroke in children with high Cerebral Blood Flow(>200cm/s) Hydroxyurea therapy, does not prevent strokes.
In general, the lower the baseline hemoglobin level in Hgb-SS persons, the higher the decline in their cognitive functions (memory, processing speed and executive functions)
Kidney
Decrease blood flow to the medulla, and infarct in the renal papilla, eventually lead to Chronic Kidney Diseases. Hgb-SS persons may have protein and blood in their urine, and marked decrease in filtration rate. The kidney can no longer concentrate urine, excrete potassium and acids. To prevent further kidney destruction, Blood Pressure control is a must, target <130/80 mmHg.
OTHER COMPLICATIONS
Priapism
About 35% of men with sickle cell disease, have prolonged and painful erections. It is related to obstruction of venous drainage of the penis.
Treatment include: aspiration of blood from the cavernous veins of the penis, and irrigating them with dilute epinephrine solution
Priapism may lead to penile fibrosis and impotence.
Foot and Leg ulcers
Leg ulcers are usually seen in 10-50 years old with sickle cell disease.
Impaired circulation leads to traumatic and sometimes spontaneous leg ulcers at the medial and lateral ankles.
Wound debridement, and bandaging with Zinc oxide impregnated bandages help.
Aplastic Crisis.
This usually occurs with Parvo b19 infections which attack the RBC precursors in the bone marrow. Folic acid deficiency and ingestion of toxins like phenylbutazone, may precipitate aplastic crisis.
Aplastic crisis is managed with blood transfusion and supportive care.
GENERAL MEASURES IN MANAGEMENT OF SICKLE CELL DISEASES.
Hgb-SS persons should avoid: Alcohol, Cigarette, marijuana, Cocaine, as well as non-prescription medications.
CHILDREN
Screening for sickle disease done at birth, followed by Hb-electrophoresis.
Penicillin prophylaxis (up to age 5 years) prevents sepsis due to streptococcal pneumonia in children
Prevnar (Pneumococcal vaccine) prevents pneumococcal infection in children
Transfusions to reduce Hb-S levels <30% prevents stroke in children with high cerebral blood flow
HYDROXYURIA. This medication
. Increases total Hb-F in sickle cell disease. Hb-F retards gelation and sickling of RBCs
(i) Effective in Reducing painful episodes,
(ii) Helpful in reducing number of Acute Chest syndromes and Sickle cell crises.
BONE MARROW TRANSPLANT.
This can CURE sickle cell disease. Not widely used.
References:




 Ejisu by-election: Aduomi warns NPP against voter intimidation
Ejisu by-election: Aduomi warns NPP against voter intimidation
 High Court orders implicated four NDA officials to present defence
High Court orders implicated four NDA officials to present defence
 Let’s all be matured, patriotic to have a peaceful election this year – Dampare ...
Let’s all be matured, patriotic to have a peaceful election this year – Dampare ...
 Mahama's administration saw thievery that knew no bounds; stole from market wome...
Mahama's administration saw thievery that knew no bounds; stole from market wome...
 GRA/SML deal: Always read the stories behind the headlines or you'd look stupid ...
GRA/SML deal: Always read the stories behind the headlines or you'd look stupid ...
 GRA/SML Contract: It takes some 'wild' boldness for a president to make this dec...
GRA/SML Contract: It takes some 'wild' boldness for a president to make this dec...
 Elisu By-election: "If you call yourself a man, boo Chairman Wontumi again" — Bo...
Elisu By-election: "If you call yourself a man, boo Chairman Wontumi again" — Bo...
 Fuel tanker driver escapes with his life after tanker goes up in flames near Suh...
Fuel tanker driver escapes with his life after tanker goes up in flames near Suh...
 Uniform change: ‘Blue and white are brighter colours’ — Kwasi Kwarteng explains ...
Uniform change: ‘Blue and white are brighter colours’ — Kwasi Kwarteng explains ...
 MoE not changing all public basic school uniforms but only newly built ones — Kw...
MoE not changing all public basic school uniforms but only newly built ones — Kw...
