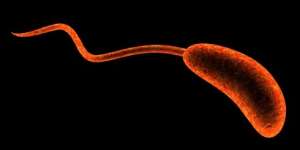
Cholera is an acute diarrheal illness, caused by ingesting the bacteria: Vibrio cholera (V. Cholera)
V. cholera are Gram-negative, comma-shaped bacteria, that live naturally, in rivers and coastal waters.
The vibrio cholera bacteria have 2 protein antigens: The H (flagella) and O (lipopolysaccharide) antigens.
Cholera bacteria are classified based on their O antigens. Currently, there are over 200 serogroups.
V. cholera biotypes, O1 and O139 are the only 2 serotypes that cause cholera epidemic or pandemic.
In Ghana, cholera epidemics, since the 1970's, have been associated with the V. cholera O1 serotypes, particularly, the El Tor, subtypes.
SOURCE OF CHOLERA:
V. cholera are found in feces of infected individuals.
Inadequate water and sewage treatment can lead to contaminated water serving as medium for person to person, transmission.
Also, dirty hands could contaminate food.
Incubation period, (time from ingestion to symptoms of disease): 24-48hours
Normally, acid in the stomach, destroys the cholera bacteria, when ingested. It requires a heavy bacterial load in the region of 1,000 to a million, bacteria in drinking water, (or 100-10,000 bacteria in food), to cause disease.
PATHOPHYSIOLOGY:
In the small intestines, the bacteria secrete toxins(enterotoxins) that lead to the following abnormalities:
1.) The toxins, cause an increase in chloride secretion, from the intestinal wall into the lumen
2.) The toxins block sodium absorption, from the lumen into the intestinal wall.
Potassium is also, lost from the body, with each bowel movement, and the greater the diarrhea, the larger the loss of potassium.
About 5% of infected persons, shall, develop severe diarrhea, vomiting and muscle cramps (muscle cramps occur when potassium is low in the body).
Unless the fluid and salts lost are adequately and rapidly replaced, dehydration occurs and severe dehydration leads to shock and death, within hours.
Case definition:
Cholera should be suspected in any community, not known for cholera, when a person, 5 years and older, suddenly, develops diarrhea and vomiting, and dies from that.
During cholera outbreaks, any person, 5 years and older, having diarrhea and vomiting, must be presumed to be having cholera.
LABORATORY DIAGNOSIS:
Stool examination shows gram negative curved rods, with single flagella.
V. cholera PCR can be used to screen stool samples.
DEHYDRATION
The diarrhea and vomiting leads to salt and water loss from the body. This condition is known as dehydration, and the clinical signs of dehydration varies with severity.
Minimal Dehydration.
The person does not look ill.
They are alert, the eyes look normal
They may be thirsty, but drink fluid in normal way.
When the skin is pinched, it gets back quickly.
Moderate Dehydration
Affected persons may be restless, irritable
Has sunken eyes
Dry mouth and tongue
Decreased urine production
They imbibe water eagerly
When their skin is pinched, the skin gets back within 2 minutes.
Severe Dehydration
Here the affected person:
Appears very weak, drowsy, or lethargic.
Very dry mouth and tongue
Pulse very fast and weak
Have sunken Eyes.
May not be able to drink water.
Skin goes back slowly, taking over 2 seconds to get back, when pinched.
MANAGEMENT OF CHOLERA INFECTION
The cornerstone for cholera treatment is adequate fluid Rehydration.
Adequate and rapid fluid rehydration (whether intravenous or oral) therapy saves life
Intravenous fluids are reserved for those with moderate to severe dehydration.
Oral rehydration is for those with initial symptoms of diarrhea and minimal to moderate dehydration
ORAL FLUIDS
During cholera infection, the enterotoxin, blocks the channels for sodium absorption. Enterotoxins do not affect the glucose channels. The glucose channels open new doors for sodium absorption when the 2 are co-administered.
All oral fluid preparations, to correct dehydration in cholera, must contain, at least, equal amount of glucose and sodium, in equivalent proportions. The more glucose, the better sodium absorption.
Normal ORS formulation, has sodium 75, chloride 65, potassium 70 bicarbonate 30, glucose 111 m.mol in l Liter of water.
I sachet ORS is added to I.0 liter of safe water.
HOME-MADE Oral Rehydration Solutions.(ORS SUBSTITUTES)
1.) 6 level tsp of sugar, and ½ tsp of salt are added to one liter of safe water.
2.) Rice water, with a little bit of added salt
3.) Millet porridge (Hausa Koko) with little bit of added salt
4.) Corn porridge (Koko) with little bit of added salt
You can add mashed banana to all the above to provide potassium supplementation
Coconut water has adequate amount of potassium, and one may drink coconut water, or add it to the home preparation of oral rehydration fluids.
Nursing mothers can continue to breastfeed their babies who have diarrhea, while waiting for medical help.
ROLE OF ANTIBIOTICS DURING CHOLERA.
Antibiotics do not prevent cholera, cholera vaccines do.
For the already infected individuals, Antibiotics may decrease the duration of the diarrhea.
Antibiotics are started when vomiting has stopped, and person adequately hydrated.
Doxycycline is frequently used as the first choice. Antibiotics are taken for 3-5 days.
Other antibacterial agents include Tetracycline, Azithromycin, and Ciprofloxacin.
(The V. cholera O1, El Tor subtypes are resistant to TMP-SMX.)
ROLE OF ZINC SUPPLEMENTS
Zinc supplements, in the form of drops, tablets, 10-20mg/day, decreases diarrhea during cholera. Zinc supplements must be taken daily until the diarrhea improves.
CHOLERA PREVENTION & CONTROL
The spread of Cholera, in a community, can be prevented by
1.) keeping fecal materials away from water and food, and
2.) killing all the cholera bacteria already present, in contaminated drinks and food, before consumption.
Always, Use Safe Water
The safest water may be Bottled water with unbroken seals.
Pipe-borne water, drinks sold in cups and bags, may not be safe and must be boiled.
Killing Vibrio cholera:
Water pathogens (bacteria, viruses, protozoa) are killed at water temperatures above 85*C, within minutes.
Boil all non-safe water. The moment water starts to boil, it is safe to drink. Let water cool naturally and store it in clean containers with covers.
Washing Hands.
N.B. 15 seconds is the minimum time, required to wash hands, adequately, with soap and running water.
Wash your hands with soap and safe water, for a minimum duration of 15 seconds.
. Before you eat,
. Before you prepare food and/or
. Before you feed others.
. Wash the hands, each time after using toilet, and
. After wiping your child's bottom, or
. After handling someone ill with diarrhea.
Edible Food
Cover all cooked food and, eat the food while it is still hot.
Avoid raw foods other than the fruits and vegetables, you have peeled.
Appropriate fecal disposal
Latrines and surfaces contaminated with feces, (including bathrooms, bedpans) must be cleaned with disinfectants, or a reconstituted solution of 1part household breach to 9 parts of water, as soon as they are soiled.
Use latrines and flush toilets to dispose of feces.
If, there is no latrine, defecate far away from rivers and streams (at least 100 feet away from water bodies) dig and bury the feces
You may defecate in polythene bags and bury them in the ground, at least 100 feet away from water bodies.
Wash hands with soap, after defecating.
Remove and wash soiled clothing, and bedding in warm or hot water. Using a washing machine is the best
Wear rubber gloves when cleaning surfaces and rooms, soiled with feces.
WHAT TO DO
If a family member develops acute watery diarrhea, start them on ORS, and seek medical attention, immediately.
CHOLERA VACCINES
3 Oral cholera vaccines are available. Individuals develop immunity, after 10 days
Sanchol and Euvichol, are vaccines, that provide immunity to V. cholera types O1, and O139
They are given to individuals older than1 year, in 2 doses, which are ingested 2 weeks apart
Vaccination provide 60% protection, for a minimum of 3 years
Dukoral is also a 2-dose vaccine (given 1 week apart), that protects against V. cholera O1.
This vaccine is administered with a buffer solution, to individual 2 years and older.
Dukoral offers 50 % protection, which may last about 2 years.
Dukoral is also administered to prevent traveler's diarrhea.




 Akufo-Addo commissions Phase II of Kaleo solar power plant
Akufo-Addo commissions Phase II of Kaleo solar power plant
 NDC panics over Bawumia’s visit to Pope Francis
NDC panics over Bawumia’s visit to Pope Francis
 EC blasts Mahama over “false” claims on recruitment of Returning Officers
EC blasts Mahama over “false” claims on recruitment of Returning Officers
 Lands Minister gives ultimatum to Future Global Resources to revamp Prestea/Bogo...
Lands Minister gives ultimatum to Future Global Resources to revamp Prestea/Bogo...
 Wa Naa appeals to Akufo-Addo to audit state lands in Wa
Wa Naa appeals to Akufo-Addo to audit state lands in Wa
 Prof Opoku-Agyemang misunderstood Bawumia’s ‘driver mate’ analogy – Miracles Abo...
Prof Opoku-Agyemang misunderstood Bawumia’s ‘driver mate’ analogy – Miracles Abo...
 EU confident Ghana will not sign Anti-LGBTQI Bill
EU confident Ghana will not sign Anti-LGBTQI Bill
 Suspend implementation of Planting for Food and Jobs for 2024 - Stakeholders
Suspend implementation of Planting for Food and Jobs for 2024 - Stakeholders
 Tema West Municipal Assembly gets Ghana's First Female Aircraft Marshaller as ne...
Tema West Municipal Assembly gets Ghana's First Female Aircraft Marshaller as ne...
 Dumsor is affecting us double, release timetable – Disability Federation to ECG
Dumsor is affecting us double, release timetable – Disability Federation to ECG
