
With the ongoing pandemic, scientists are in a rush to develop an effective vaccine to tackle the coronavirus as it appears to be our only way of dealing with the ongoing threat. The process of vaccine testing was not helped with the recent comments from two French scientist/doctors who were discussing the potential testing of newly developed vaccines on Africans. These comments caused an outburst amongst the African community online with some of our prominent politicians condemning the comments made by the two French doctors.
Is our fear of a potential coronavirus vaccine justified or does the fear stem from our lack of knowledge on the types of vaccine, the safety and danger of a vaccine, the different stages involved in vaccine production before a vaccine can be used in a clinical trial?
This article aims to educate the public on what vaccine entails, the different types of vaccine and the stringent measures involved in a vaccine trial before a vaccine can be tested on human.
What are the different types of vaccine?
There are several different types of vaccines with each type designed to teach our immune system how to fight off certain kinds of germs. The most common types of vaccines are live-attenuated vaccines, inactive vaccines, subunit, recombinant polysaccharides, conjugated vaccines and toxoid vaccines. Other emerging vaccines which are less common are DNA vaccines, recombinant vector vaccines and many more.
Live-attenuated vaccines: In the context of the coronavirus, the virus will be weakened or its harmful effect will be reduced significantly to the point where they are confident that under no circumstance can the virus be revived in the body when the weakened virus is given to an individual. Using a fly as an analogy, if the fly is the virus, the whole fly will be weakened to such extent that it cannot fly, walk or move but it is still alive. Because this type of vaccine is similar to someone actually catching the virus, your body creates strong and long-lasting immune response that will give you a lifetime protection against the coronavirus. This is the reason why people who have recovered from the coronavirus are unlikely to get sick by the same strain of coronavirus twice.
The disadvantage of this virus is that people with already weakened immune systems, long-term health problems, or people who’ve had an organ transplant will not be allowed to receive this vaccine as their body will not be able to fight of the weakened, reduced or less harmful coronavirus. Keep in mind that although this vaccine is weakened, it is still a live vaccine that can cause harm if given to immune-compromised patients. Moreover, there is always a small chance that the virus can be revived in the human body if not weakened properly, transported properly or introduced in the right circumstance or right dose. In any clinical trial, there is always the probability of things going wrong particularly in clinical trial phase one when a new compound is being introduced to the human body for the first time especially a live virus.
Inactive vaccines: Inactivated vaccines make use of the killed version of the coronavirus instead of a live or weakened virus. Using the fly analogy again, the fly is killed before use. The disadvantage of this type of vaccine is that the vaccine usually does not provide immunity or protection as strong as the live vaccine. The inactive vaccine carries no risk of inducing the disease however inactive vaccine may not always induce an immune response, but even if it induces immune response, the response might not be long-lived. Moreover, the vaccine is usually given in two different doses as a booster shot in order to prolong immunity against the coronavirus. An example of an inactive vaccine that has been used for many years includes Hepatitis A, Polio and Rabies vaccine.
Toxoid vaccines: In the context of the coronavirus, this type of vaccine uses a toxin (harmful product) made by the coronavirus that causes the disease. Using the fly analogy, a product of the fly or the toxic compound released by the fly that causes the disease is used as a vaccine. So in essence, your body creates immunity to the part of the coronavirus that causes disease instead of the virus itself. This means that the immune response is targeted to the toxin instead of the whole germ. With these types of vaccine, a second shot called a booster is required to ensure a prolonged protection to the virus. Toxoid vaccines that are currently used are Diphtheria and tetanus. Toxoid vaccines are safe because the vaccine antigens are not actively multiplying and do not spread to unimmunized individuals. This type of vaccine is stable as it is less susceptible to changes in temperature, humidity and light, but more importantly, unlike live or attenuated vaccine, this vaccine cannot cause the disease that it is designed to prevent.
Subunit, recombinant, polysaccharide, and conjugate vaccines: In the context of the coronavirus the vaccine makes use of a small part of the coronavirus such as its protein spikes. Because this vaccine uses only specific pieces of the coronavirus, they give a very strong immune response that’s targeted to key parts of the coronavirus. Using the fly analogy, it’s like using the leg of the fly as a vaccine so your immune system only recognises the leg and not the other area of the fly such as the wings, head, eyes, etc. They can also be used on almost everyone who needs them, including people with weakened immune systems and long-term health problems because they don’t contain live component. limitations of these vaccines is that the precision in manufacturing this type of vaccine comes at a cost as the pathogen must be examined in detail to determine which particular combination will produce an effective immune response. Most of the time, a response can be elicited but there is no guarantee immune memory will be made. Without immune memory, the whole point of vaccination is meaningless. Moreover, you may need booster shots to get ongoing protection against diseases. Subunit, recombinant, polysaccharide, and conjugate vaccines currently being used are hepatitis B, shingles and many more.
Some of these types of vaccines such as (toxoid vaccine) cannot be considered for the coronavirus. Therefore to select the type of vaccine that will be used, a variety of factors are considered which is ultimately based on the make-up of the virus, the toxicity of the virus, safety of the vaccine, how the virus infect the human body, etc.
So how tightly regulated are vaccine trial?
Before a vaccine is ever recommended for use, it’s tested in laboratory. This process can take several years. In America, FDA uses the information from these tests to decide whether to test the vaccine with people. However, because there is an urgent need for COVID-19 vaccine, the aim is to develop a vaccine within 12-18 months. Does this mean that scientist will need to cut corners to meet the high demand of developing a vaccine? And what is the increase risk for volunteers for these clinical trials? First, let me explain the different types of vaccine stages.
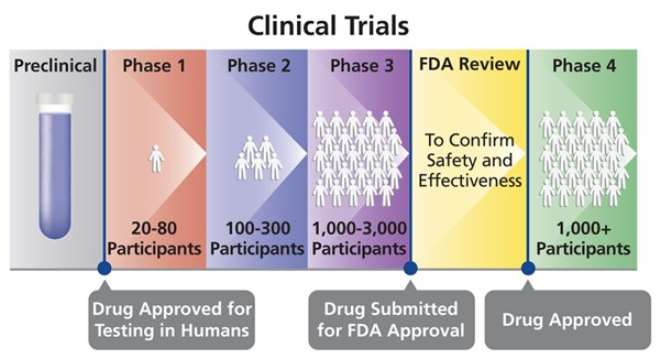
The preclinical phase involves all the work that goes on in laboratories to develop a vaccine. The aim of this phase is to identify (discovery) relevant antigens (e.g. screening), to create a vaccine concept, to evaluate vaccine efficacy (effectiveness) in test tubes and on animals and to manufacture the vaccine to Good Manufacturing Practice standards before the vaccine can enter into clinical trial phases. Out of 100% potential vaccines developed in a laboratory, only 0.1% of all potential vaccines created in a laboratory are approved for use in clinical trials. This is a very small fraction which further shows the rigorous screening process vaccines go through.
Phase I clinical trials are small-scale trials to assess whether the vaccine is safe in humans and what immune response it evokes. For diseases of poverty, this covers trials in European volunteers (phase Ia) and then in populations in Developing Countries (phase Ib).
Phase II clinical trials are larger and look mainly to assess the efficacy of the vaccine against artificial infection and clinical disease. Vaccine safety, side-effects and the immune response are also studied.
Vaccines that progress to phase III clinical trials are studied on a large scale of many hundreds of subjects across several sites to evaluate efficacy under natural disease conditions. If the vaccine retains safety and efficacy over a defined period, the manufacturer is able to apply to the regulatory authorities for a licence to market the product for human use.
The final phase IV happens after the vaccine has been licensed and introduced into use. Also called post-marketing surveillance, this stage aims to detect rare adverse effects as well as to assess long term efficacy.

Every licensed and recommended vaccine goes through years, sometimes up to 10 years of safety testing including: testing and evaluation of the vaccine before it’s licensed by the Food and Drug Administration (FDA) and recommended for use by the Centers for Disease Control and Prevention (CDC), monitoring the vaccine’s safety after it is recommended for infants, children, or adults. During a clinical trial, a vaccine is tested on people who volunteer to get vaccinated. These tests answer important questions like: Is the vaccine safe? What dose (amount) works best? How does the immune system react to it? Throughout the process, FDA works closely with the company producing the vaccine to evaluate the vaccine’s safety and effectiveness. All safety concerns must be addressed before FDA licenses a vaccine.
Moreover, a range of vaccine health and safety organisations such as: Vaccine Adverse Events Reporting System (VAERS), The Vaccine Safety Datalink (VSD), Post-licensure Rapid Immunization Safety Monitoring System (PRISM), Clinical Immunization Safety Assessment Project (CISA) ensure that all vaccines meet the safety standard.
So what are the actual advances currently made to produce a vaccine for the coronavirus?
On 18 March, a trial of a different recombinant COVID-19 vaccine was registered. That vaccine is based on adenovirus Type 5 Vector (currently called Ad5-nCoV), and is recruiting 108 adults in China. A Phase 2 randomized trial beginning 12 April was subsequently registered for this vaccine. That trial is aiming to enrol 500 participants, in 3 arms: 250 receiving a middle dose, 125 a low dose, and 125 a placebo injection, with 6 months follow-up.
Scientists from Oxford University are also fast-tracking another adenovirus vector vaccine (new type of vaccine), called ChAdOx1 nCoV-19. They are leap-frogging straight to a Phase 1/Phase 2 trial and hope to beat the 12-18 months estimate till a vaccine is available. On 27 March, they announced that they are recruiting participants 510 healthy people, with 260 to be randomized to the vaccine and the other 250 to a saline injection. It will be a 6-month trial, and although they are already recruiting, preclinical animal testing is still going on.
Thirdly, according to the company manufacturing it, the first dose of this trial was given to a healthy volunteer on 6 April 2020. Currently called INO-4800, this one is partly funded by the Gates Foundation, and it builds on previous work on a vaccine for another coronavirus, MERS. This Phase 1 trial aims to recruit 40 people, at 2 sites in the US: Philadelphia and Kansas City, with 6 months follow-up (to November 2020).
These types of new vaccines using adenovirus base human vaccine, stand out as they have been developed against adenovirus type 4 and 7, administered orally to military recruits to decrease the number of acute respiratory diseases. This type of vaccine was very effective and had a long-lasting immunity and was considered extremely safe with only 2 out of 200000 developing vaccine-related symptoms.
Though this type of vaccine is considered safe, the fact that vaccine production normally takes years (10 years in some cases) and are subject to rigorous scrutiny by a range of health and safety organisations, raises questions that the public should be able to obtain answers to. Is it ethical to subject healthy individuals to vaccines that have been manufacture in the lab within just 5 months? Is the fast tracking of these vaccines mainly as a result of overworked scientists who are prioritizing the cure for the coronavirus over everything? Or is the fast track as a result of health and safety organisations overlooking certain safety measures which would be important to address under any normal (non-pandemic) circumstance?
Is this the case of sacrificing the few for the many? Or are scientist extremely confident in the safety of this type of vaccine and are certain that they do not come with any detrimental risks?
Regardless of the type of vaccine currently being manufacture, these strict rules were implemented for a reason (with reference to the elephant man clinical trial in UK 2006). The only way the public, not just Africans, the public will trust theses vaccines will be in a situation where transparency and public education is practice. I am not talking about transparency by uploading data on the progress of the vaccine online with the expectation that the public conduct their own research to first: find these information and second, attempt to actually understand what these data mean. I am talking about regular public announcement from scientist and health and safety organisations involved in the vaccine production, explaining the progress of the vaccine, their concerns, advantages, disadvantages, setbacks in lay language. After all, this is a pandemic.
I hope that this information somehow gives you a clear understanding of what vaccines are, the different phases and stages involved so that you can make your own informed decision as to whether to accept or trust the vaccines.
By Dr Marian Manso (PhD)




 Akufo-Addo’s govt is the ‘biggest political scam’ in Ghana’s history – Mahama ja...
Akufo-Addo’s govt is the ‘biggest political scam’ in Ghana’s history – Mahama ja...
 Performance Tracker is not evidence-based — Mahama
Performance Tracker is not evidence-based — Mahama
 Four arrested for allegedly stealing EC laptops caged
Four arrested for allegedly stealing EC laptops caged
 $360 million IMF bailout not enough for Ghana – UGBS Professor
$360 million IMF bailout not enough for Ghana – UGBS Professor
 Shrinking Penis Allegations: Victim referred to trauma hospital due to severity ...
Shrinking Penis Allegations: Victim referred to trauma hospital due to severity ...
 Adu Boahen Murder: Case adjourned to May 9
Adu Boahen Murder: Case adjourned to May 9
 ‘I've health issues so I want to leave quietly and endure my pain’ — Joe Wise ex...
‘I've health issues so I want to leave quietly and endure my pain’ — Joe Wise ex...
 Let’s help seek second independence for Ghana before NPP sells the country – Law...
Let’s help seek second independence for Ghana before NPP sells the country – Law...
 New Force aims to redeem Ghana and West Africa — Nana Kwame Bediako
New Force aims to redeem Ghana and West Africa — Nana Kwame Bediako
 ‘I didn't say I would buy Ghana if voted against; I said I’ll buy it back from f...
‘I didn't say I would buy Ghana if voted against; I said I’ll buy it back from f...
