After six long weeks of hospital admission, blood transfusions, and an antibiotics bill in excess of GH₵3,000 (US$750), we confirmed that the cause of 4-year-old Mansa's (not her real name) unsettling fever and bone pain was cancer of the blood (Leukemia). During this same period, Mansa's mother succumbed to kidney failure in the same hospital. The entire extended family had spent their entire fortune in the hope of keeping both mum and daughter alive.
So, we broke the news of Mansa's diagnosis including the estimated out-of-pocket expenditure (GH₵20,000 for 3 years of treatment) to dad first and then, to the rest of the family (on dad's request). One member of the family made this remark during the counselling session: “Cancer?! In this child, then why bother the doctor? She's going to die anyway”. They missed their first clinic appointment after this; Mansa died at home the following week and subsequently captured as yet another reported death from childhood cancer in Ghana. Stark reality
Eighty percent, 80% of all children diagnosed with cancer live in resource-limited countries of Africa and South America. In the developed world, 85% of childhood cancers are curable! That is, 8 to 9 out of 10 kids diagnosed with cancer as in Mansa's case, will be cured of their cancer and be alive 5 years or more after completing treatment.
In Ghana, the two main teaching hospitals together see about 400 (out of an expected 1300) new reported cases of childhood cancer annually. About a third of these kids will die; another third will not complete their treatment (abandon treatment) and eventually die; and the final third will survive.
Let's put this in context: in developed countries, 4-year-old Mansa would have been diagnosed within 3 days of admission; she would most likely be alive now no matter the cost and most likely, the high out-of-pocket expenditure would not have been a key consideration for the family in opting not to treat Mansa; thus choosing death over life. What does it take to cure a child of cancer?
Half a century ago there were many 'Mansas'in the now developed nations. Leukaemia or cancer diagnosis meant certain death; it was a matter of how long. This is the situation in most cases in Ghana now. So, how did they do it, and continue to do it in the advanced countries?
Collaborative Research:
National and international collaborations between various childhood cancer treatment centers to improve diagnostic and treatment strategies; including training and retraining of experts in the field of childhood cancer management
Advocacy:
Largely led by private individuals and non-governmental, not-for-profit organizations that run effective campaigns to create awareness and raise funds to support the treatment of childhood cancers. Can individual entities including families, private organizations, or even government alone bear the huge financial burden of curing childhood cancers?
Health Infrastructure:
Curing a childhood cancer requires effective healthcare systems (data systems; allied health systems; diagnostic systems) including infrastructure and constant updating of existing knowledge, in addition to highly trained human resource in sufficient numbers.
Political Will:
The government must commit sustainable human and financial capital through sustainable, long term policies; establishing more centers of excellence dedicated to childhood cancer care; and training adequate experts in the field to ensure true universal health coverage Food for thought:
- When will our National Health Insurance Authority recognize the need for including least part of the cost of the treatment of even the commonest childhood cancer in Ghana in its benefits package?
- What would you prefer as a citizen: your taxes of GH₵20,000 (US$5,000) spent in:
- Curing (with 100% certainty) 20 children with even the deadliest form of malaria; or
- providing treatment for Mansa who has realistically, a 30%chance of surviving in Ghana?
- Will another Mansa, born to parents of low socioeconomic class and living in Asante-Akim Agogo, be able to beat leukaemia in the next 50 years in Ghana?
- Will you vote for the person who provided you with good motorable roads or the one who invested in childhood cancer research?

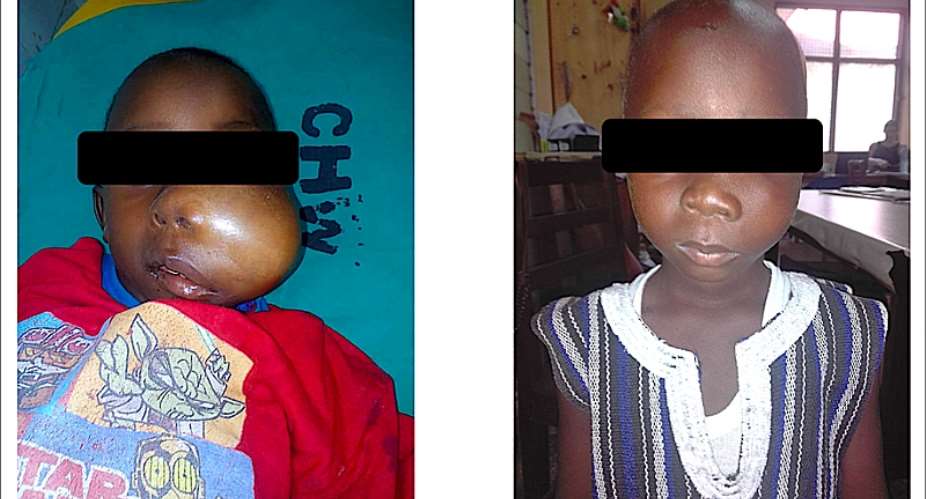
Photo: A child with Burkitt Lymphoma, a common blood cancer in Ghana – Before and After Treatment. He was treated with cheap anti-cancer medicines over a period of 8 months. The overall cost of treatment was less than a tenth of the cost of treating breast cancer. Breast cancer treatment is covered by NHIS but Burkitt Lymphoma is not covered.
---citinewsroom




 2024 election will be decided on the grounds of the economy; choice of running m...
2024 election will be decided on the grounds of the economy; choice of running m...
 Dumsor: We're demanding less; just give us a timetable — Kwesi Pratt to ECG
Dumsor: We're demanding less; just give us a timetable — Kwesi Pratt to ECG
 Do I have to apologise for doing my security work, I won’t – Simon Osei-Mensah r...
Do I have to apologise for doing my security work, I won’t – Simon Osei-Mensah r...
 Prestea and Bogoso mines: Complete payment of outstanding salaries not later tha...
Prestea and Bogoso mines: Complete payment of outstanding salaries not later tha...
 NDC postpones Prof. Opoku-Agyemang entry tour to May
NDC postpones Prof. Opoku-Agyemang entry tour to May
 All my businesses have collapsed under Akufo-Addo — NDC Central regional chair
All my businesses have collapsed under Akufo-Addo — NDC Central regional chair
 Military, Prison Officers clash in Bawku, three injured
Military, Prison Officers clash in Bawku, three injured
 GRA-SML contract: MFWA files RTI request demanding KPMG report
GRA-SML contract: MFWA files RTI request demanding KPMG report
 Court threatens to call second accused to testify if NDC's Ofosu Ampofo fails to...
Court threatens to call second accused to testify if NDC's Ofosu Ampofo fails to...
 Family accuses hospital of medical negligence, extortion in death of 17-year-old...
Family accuses hospital of medical negligence, extortion in death of 17-year-old...
