The rising Covid-19 wave in India has affected the country's healthcare system with a large number of doctors and health workers testing positive for the coronavirus disease.
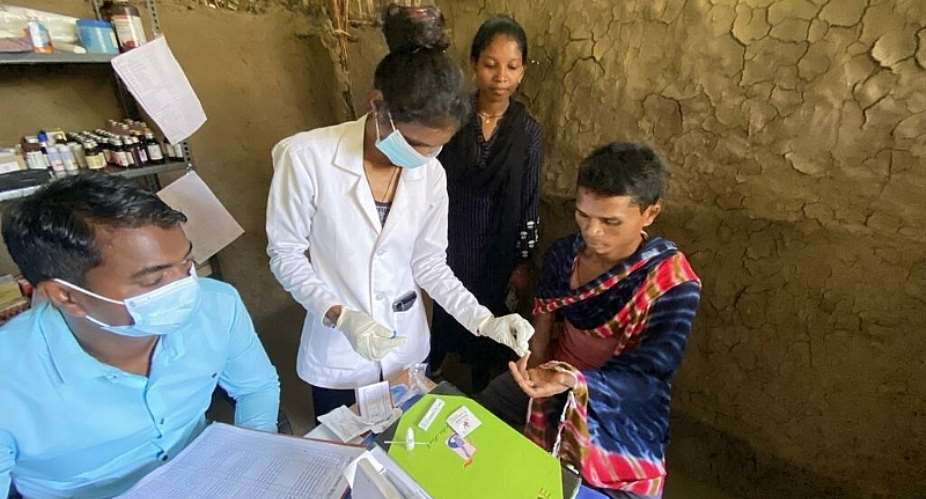
Manju Kumari, 49, an accredited social health activist (ASHA) worker, is a foot soldier among India's million-strong frontline healthcare workers that survey populations to find suspected Covid cases, and monitor patients' oxygen and temperature levels daily.
“I have tested positive and will not be able to carry out my duties. I will have to recover,” Kumari told RFI, pointing out that many of the 6,500 ASHA workers in New Delhi were affected.
Though various studies have found that a third dose of vaccine can provide enhanced protection against hospitalisation from infection by the Omicron variant, many health staff will not be able to take the booster shots immediately due to recent infections.
Staff crunch
With the Omicron-driven Covid surge, many doctors and healthcare workers have contracted the disease, a majority of them for the second time. Infection has been particularly high in the metropolitan cities.
India has seen an exponential rise in coronavirus cases over the past week. From fewer than 10,000 daily cases a fortnight ago, the country is witnessing an alarming spread of the virus, recording more than 200,000 cases daily.
Daily infections rose sharply on Thursday with 317,532 cases registered in the last 24 hours, which pushed the caseload to over 38 million, according to health ministry data.
About 70 percent of the eligible population has received two primary vaccines doses and a booster campaign for health workers and at-risk population is underway.
At the global level, India is the second worst-hit country after the US. In the capital, nearly 800 doctors as well as nurses and paramedics from the six major hospitals in Delhi are ill with Covid.
Though most of them have mild symptoms and are in home isolation, the workforce has been depleted, resulting in hospitals having to curtail routine clinics and surgeries.
Hospitals in Mumbai are also faced with a shortage of staff as several doctors, nurses and other healthcare workers across public and private facilities have been infected with the coronavirus.
This includes major hospitals like King Edward Memorial, Lokmanya Tilak Medical Hospital and St George's Hospital that are reporting a staff shortage of anywhere between 5 to 30 percent.
The Maharashtra Association of Resident Doctors on Sunday reported that more than 300 resident doctors have tested positive for Covid in the state so far.
Though the country's healthcare system has been prepped up before the current wave, it was already short-staffed in health care.
India has about 17 active health workers that includes doctors, nurses and midwives per 10,000 people, according to the Indian Institute of Public Health and the World Health Organization (WHO).
That number is far below the WHO's threshold of 44.5 trained health workers per 10,000.
City hospitals affected
Since the pandemic hit India in March 2000, 1,492 doctors have died with 270 doctors alone succumbing in the second wave of the coronavirus disease in April-May last year.
“Yes, it is a matter of concern and we are addressing this problem using all available resources,” the Indian Medical Association national president J A Jayalal told RFI.
In south India, the healthcare system has also been hit hard. Major government Covid hospitals in capital Chennai are witnessing clusters among their medical staff.
The Tamil Nadu government has issued new guidelines for triage and treatment of Covid patients. This is to prevent patients who could be treated under home isolation from reaching major health care facilities, and save hospital resources to treat serious cases.
Hospital authorities say that healthcare workers have been testing positive routinely, but they began seeing a higher number of infections starting the last week of December.
“Frontline workers are bound to have more infections as we are in a middle of a wave driven by a highly transmissible variant," Dr Shashank Joshi, a member of the Covid-19 task force, told reporters last week.
"It is important for hospitals to wait for a negative RT-PCR test before calling the doctors back on duty.”
Though hospitals have scaled up capacity to accommodate the increasing number of Covid patients and are recruiting more healthcare staff, doctors, nursing staff and other frontline workers are increasingly staying away from work for at least a fortnight after contracting the virus.




 Former Kotoko Player George Asare elected SRC President at PUG Law Faculty
Former Kotoko Player George Asare elected SRC President at PUG Law Faculty
 2024 elections: Consider ‘dumsor’ when casting your votes; NPP deserves less — P...
2024 elections: Consider ‘dumsor’ when casting your votes; NPP deserves less — P...
 You have no grounds to call Mahama incompetent; you’ve failed — Prof. Marfo blas...
You have no grounds to call Mahama incompetent; you’ve failed — Prof. Marfo blas...
 2024 elections: NPP creates better policies for people like us; we’ll vote for B...
2024 elections: NPP creates better policies for people like us; we’ll vote for B...
 Don’t exchange your life for wealth; a sparkle of fire can be your end — Gender ...
Don’t exchange your life for wealth; a sparkle of fire can be your end — Gender ...
 Ghana’s newly installed Poland train reportedly involved in accident while on a ...
Ghana’s newly installed Poland train reportedly involved in accident while on a ...
 Chieftaincy disputes: Government imposes 4pm to 7am curfew on Sampa township
Chieftaincy disputes: Government imposes 4pm to 7am curfew on Sampa township
 Franklin Cudjoe fumes at unaccountable wasteful executive living large at the ex...
Franklin Cudjoe fumes at unaccountable wasteful executive living large at the ex...
 I'll 'stoop too low' for votes; I'm never moved by your propaganda — Oquaye Jnr ...
I'll 'stoop too low' for votes; I'm never moved by your propaganda — Oquaye Jnr ...
 Kumasi Thermal Plant commissioning: I pray God opens the eyes of leaders who don...
Kumasi Thermal Plant commissioning: I pray God opens the eyes of leaders who don...
